Multilocular Simple Bone Cyst of the Mandible: Part 2: Histopathologic Appearance and Brief Review of the Literature
March 31, 2021
https://doi.org/10.23999/j.dtomp.2021.3.3
J Diagn Treat Oral Maxillofac Pathol 2021;5:36–42.
Under a Creative Commons license
HOW TO CITE THIS ARTICLE
Nozhenko OA, Snisarevskyi PP, Zaritska VI. Multilocular simple bone cyst of the mandible: part 2: histopathologic appearance and brief review of the literature. J Diagn Treat Oral Maxillofac Pathol 2021;5(3):36–42.
Contents: Summary | Introduction | Case | Discussion | Conclusion | Author Contribution | References (24)
SUMMARY
The purpose of this report is to highlight the histopathologic appearance of the mandibular simple bone cyst (SBC) – a pathologic condition which continues to stay an enigma for a lot of colleagues. Cone-beam computed tomography of a two-chamber SBC (ie, multilocular type) of the mandibular body in a 41-year-old white female is analyzed. Brief literature review is also performed giving the possibility to understand all intraoperative appearances of the SBCs and contemporary techniques of its management.
INTRODUCTION
Simple bone cyst (SBC) is an intraosseous pseudocyst (ie, nonepithelial–lined bone cavity)1 which may be uni- or multilocular.2 Rudolf Virchow was a first one who recognized the SBCs in the long bones and published the report “About the formation of bone cysts” in 1876.3 Such type of cysts located in a jaw bone was first discussed by Carl Lucas in the report of Theodor Blum in 1929 where traumatic injury was determined as causative factor.4
The SBC belongs to one of four types of jaws` pseudocysts5:
-
Aneurismal (haemorrhagic-aneurismal)6 bone cysts.
-
Traumatic (ie, simple) bone cysts.
-
Static bone cysts (ie, Stafne`s bone defects).
-
Focal osteoporotic bone marrow defect.
SBC is named in the literature as hemorrhagic bone cyst,7,8 traumatic cyst,9 extravasation cyst,10 progressive bone cavity,11 solitary bone cyst12, idiopathic bone cavity,13 and single-chamber bone cyst14.1 Tymofieiev terms such type of cyst as a sheathless (ie, capsuleless) cyst (synonym: post-traumatic cyst).15
According to Olvi et al SBCs involve extra-maxillofacial bones in the next distribution: proximal humerus (in 50 percent), proximal femur (in 25 percent), and proximal tibia.16 That statistics proves the fact that in 90 percent the SBCs involves metaphysis of the long bones.17
In the first part of our work2 we presented the data of a 41-year-old white female with a multilocular type of mandibular SBC. Consecutive cone-beam computed tomography (CBCT) scans and surgical technique were analyzed.2
The purpose of this report is to highlight the histopathologic appearance of the mandibular SBC – a pathologic condition which continues to stay an enigma for a lot of colleagues.17
CASE
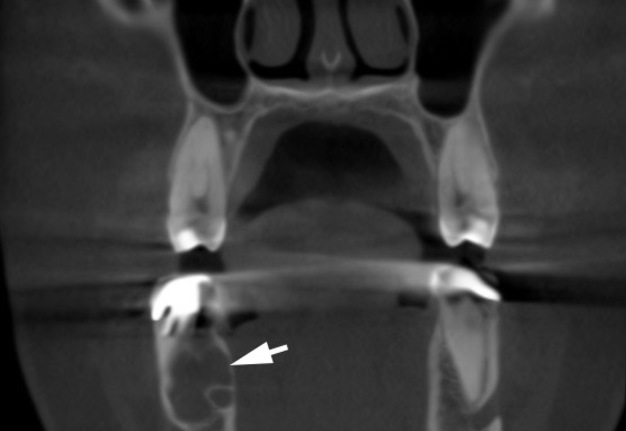
A 41-year-old white female with a two-chamber SBC (ie, multilocular type) of the mandibular body (ie, corpus) was treated in the Center of Maxillofacial Surgery.2 The preliminary diagnosis was confirmed by anamnesis, CBCT data (Fig 1), vitality of the involved teeth, and asymptomatic course.2
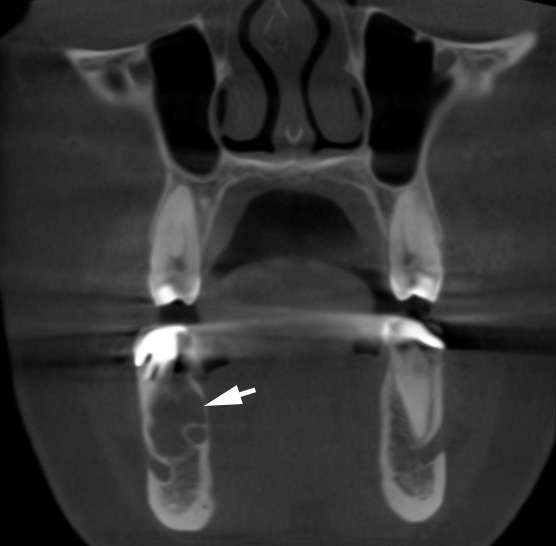
Firstly, a biopsy was performed in the area of anterior bony chamber of the cystic lesion and a 1.0 ml of serous fluid was obtained after trepanation of buccal cortical plate. Specimen was received by curettage of the bone walls of the intraosseous cavity. Histology showed blood clots in the huge areas of fibrous tissue and collagen.2 A 5-month follow-up CBCT demonstrated complete fulfillment of the anterior chamber by a new bone tissue (Fig 2).
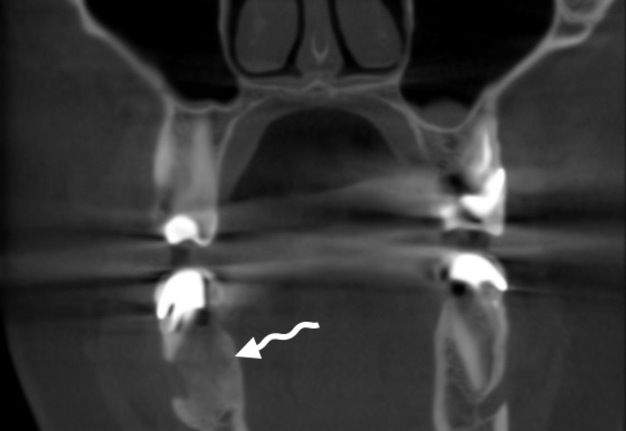
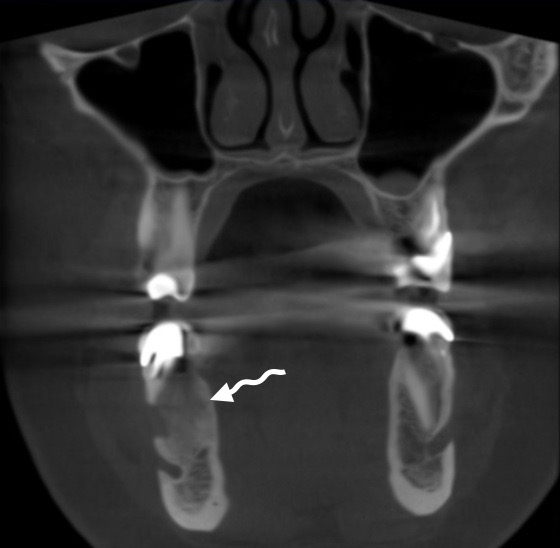
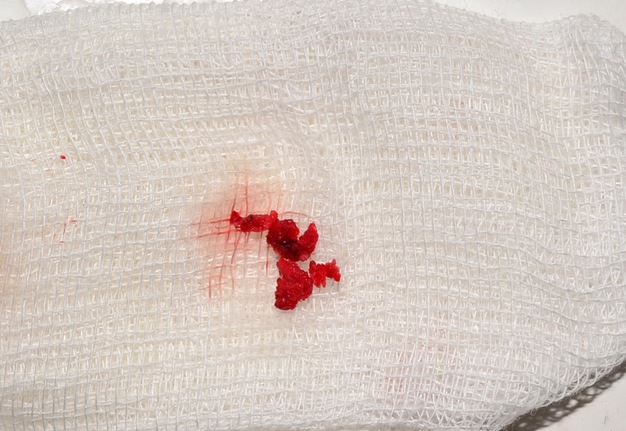
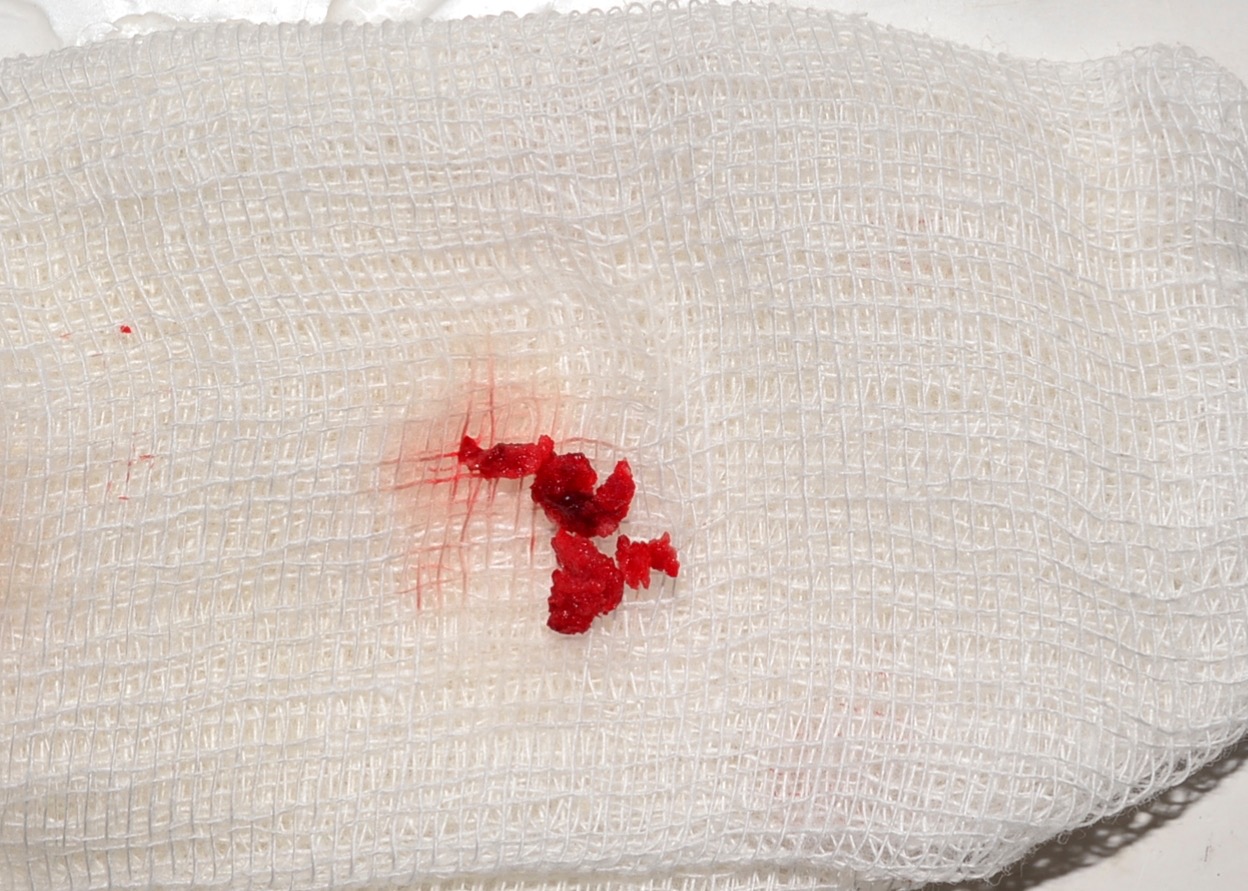
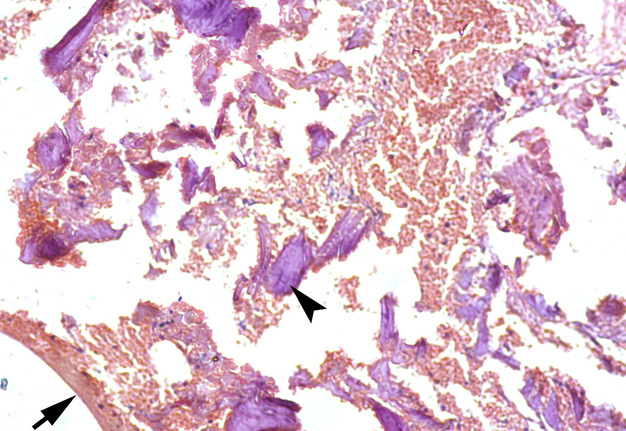
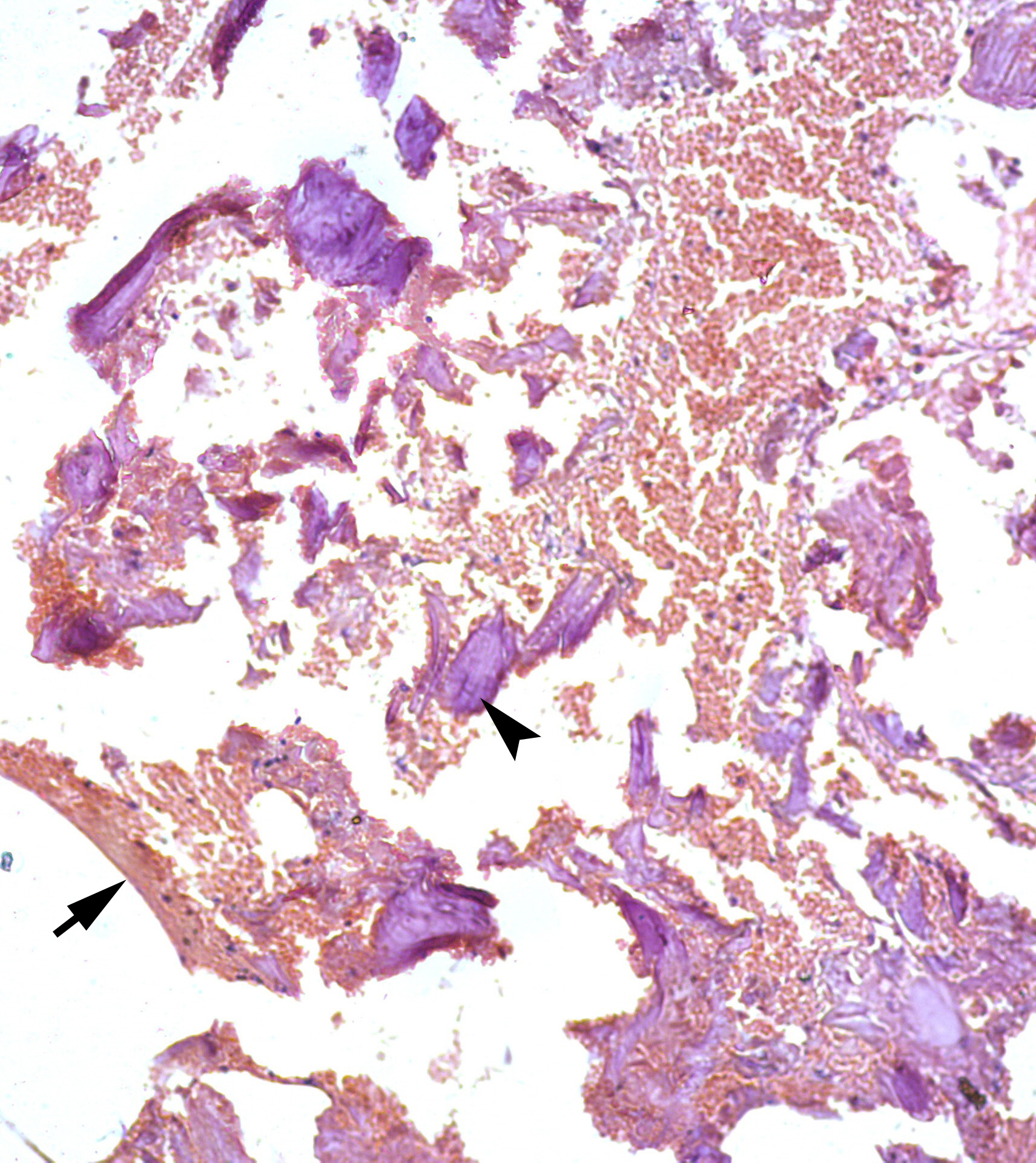
Second surgery included curettage of the posterior chamber of the cyst (where a small sponge bone particles were obtained) (Fig 3) and bone grafting with xenograft (BIO-GEN® MIX [cancellous-cortical] Bioteck S.p.A., Vicenza, Italy). Histopathological examination revealed the appearance similar to the appearance presented in the study of Xanthinaki et al (reported a 25-year-old white female with a SBC of the ramus),18 and showed the parts of vascular connective tissue and bone spicules (Fig 4).
DISCUSSION
SBCs is a rare clinical entity reaching only 1.05 percent among all jaw cysts.19 Multilocular type of SBCs is even more rare and counts from 6.38 to 26.92 percent of total number of SBCs.20,21
Already published multichamber variants of SBCs showed that the single-chamber bone cyst term cannot be applied to all SBCs as the published data and our case are proving the existence of two types of SBCs – uni- and multilocular.
You et al in 2017 analyzed 30 idiopathic bone cavities (ie, SBCs); and their study revealed next distribution of 30 idiopathic bone cavities in 27 patients:13 in 13 cases the cysts localized in the right posterior mandible, in 11 cases – in the left posterior mandible, in 5 cases – in symphyseal area, and only in one case the cyst was found at the left lateral maxilla.13 Thus, our case proves the majority cases data of You et al, in which SBCs were localized in the right posterior mandible.
Pseudocystic histological features of the SBCs have been proved by numerous publications. Discussion of twenty-two cases and treated by curettage in the study of Demirbas et al had shown next histopathological findings: loose connective tissue (n = 3 [13.6 percent]), empty (n = 16 [61.5 percent]), fluid content (n = 4 [18.1 percent]), and osseous-like tissue (n = 3 [13.6 percent]).19
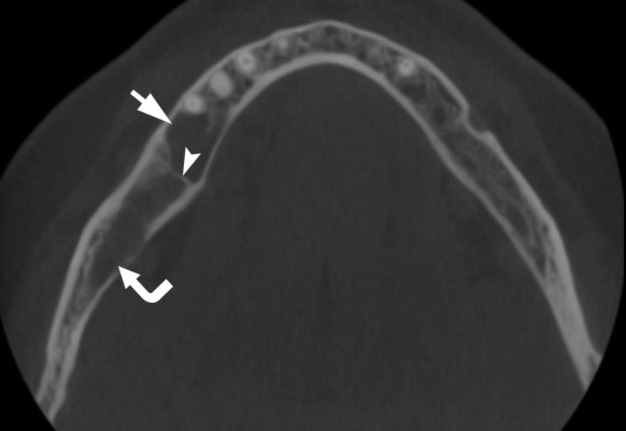
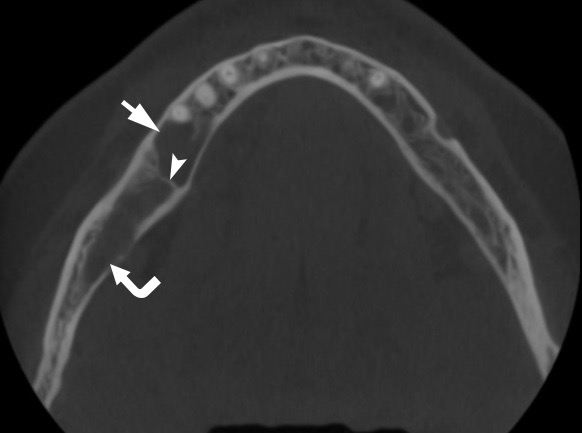
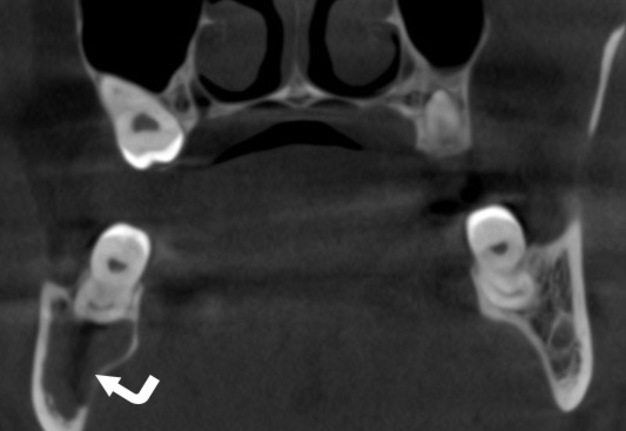
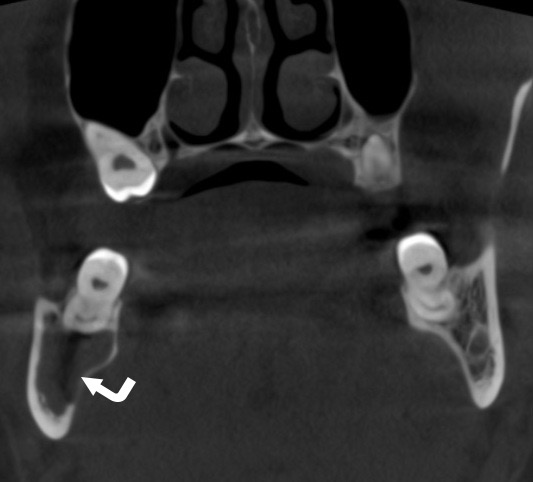
FIGURE 1A. Axial (A) and coronal (B) CBCT scans of a 41-year-old white female with a multilocular SBC of the right mandible. The bone septa (arrowhead) divides the pseudocyst into anterior (arrow) and posterior (curved arrow) camera (ie, chamber). Printed with permission and copyrights retained by O.A.N.
FIGURE 1B. Axial (A) and coronal (B) CBCT scans of a 41-year-old white female with a multilocular SBC of the right mandible. The bone septa (arrowhead) divides the pseudocyst into anterior (arrow) and posterior (curved arrow) camera (ie, chamber). Printed with permission and copyrights retained by O.A.N.
FIGURE 4. A 41-year-old white female with a multilocular type of SBC of the right mandible. Histological appearance, similar to the appearance presented in the study of Xanthinaki et al (reported a 25-year-old white female with a SBC of the ramus),18 showed the parts of vascular connective tissue (arrow) and bone spicules (arrowhead) (hematoxylin and eosin stain, original magnification × 10). Printed with permission and copyrights retained by V.I.Z. and P.P.S.
Bimaxillary SBC case (two – intramandibular cysts and one – intramaxillary cyst) of Saldaña et al macroscopically revealed samples of liquid content, bone tissue and cavity membranes, and microscopically – fibro-cellular wall with highly vascularized areas, multi-nucleated giant cells mainly in areas of hemorrhage.14
Xanthinaki et al inside the cavity of the intramandibular SBC have found only extremely thin layer of connecting tissue and only in some places.18
SBC in the paper of Velasco et al which showed the cystic evolution (growth after first surgery) contained mild haematogenous liquid and histologically presented vital lamellar bone tissue and recent hemorrhage areas.22
Despite the report of Matsuda et al presents the floating inferior alveolar neurovascular bundle in a large SBC involved mandibular body, in our case the bundle was just displaced inferiorly.23
The article by Chell et al should be a warning to physicians who have cases of SBCs because the mandibles weakened by such asymptomatic cysts may become more prone to fractures.24
Treatment options for SBCs are perfectly described in a recent orthopedic and oral-maxillofacial surgery works.2,20 Three management strategies for jaws` SBCs became the most popular: 1) bone perforation and stimulation of blood clot formation, 2) curettage of the cavity and flap repositioning and suture, 3) decompression and warm saline solution irrigation.2
In our case we combined two surgical techniques in two separated chambers of the SBC. Both techniques showed efficacy in fulfillment of the cystic cavities and can be recommended for the usage in similar cases giving preference to the surgical exploration and gentle curettage.13
CONCLUSION
The simple bone cyst as an asymptomatic intraosseous pseudocystic entity is proved to be effectively managed applying different strategies, giving minimally invasive techniques a clear priority. Histopathological findings of the simple bone cysts` specimens are well-documented and leave no space for possible malignization of such types of cyst due to the absence of true cystic lining.
AUTHOR CONTRIBUTION
Conceptualization: Nozhenko OA.
Data and interpretation acquisition: Nozhenko OA, Snisarevskyi PP, Zaritska VI.
Drafting of the manuscript: Nozhenko OA.
Critical revision of the manuscript: Snisarevskyi PP, Nozhenko OA, Zaritska VI.
Approval of the final version of the manuscript: all authors.
REFERENCES (24)
-
Rattana P. Simple bone cyst of the anterior mandible: a case report. JOJ Case Stud 2017;4(1):555626. Crossref
-
Nozhenko OA, Zaritska VI, Snisarevskyi PP, Fesenko II. Case report: multilocular type of mandibular simple bone cyst. Part 1: cone beam computed tomography (CBCT) findings, revision of the synonyms and treatment strategies. J Diagn Treat Oral Maxillofac Pathol 2018;2(4):179−85. Crossref
-
Virchow RLL. Über die Bildung von Knochencysten. Acad Mber 1876;369–81.
-
Lucas CD: Discussion. In Blum T: Do all cysts of the jaw originate from the dental system? J Am Dent Assoc 1929;16(4):647−61. Crossref
-
Regezi JA, Sciubba JJ, Jordan RCK. Oral pathology. 7th ed. Cysts of the jaws and neck. St. Louis, Missouri: Saunders 2017. 245−68.
-
Grecchi F, Zollino I, Candotto V, Gallo F, Rubino G, Bianco R, Carinci F. A case report of haemorrhagic-aneurismal bone cyst of the mandible. Dent Res J (Isfahan) 2012;9(Suppl 2):S222–4. Link
-
Howe GL. 'Haemorrhagic cysts' of the mandible. I. Br J Oral Surg 1965;3(1):55–76. Crossref
-
Howe GL. 'Haemorrhagic cysts' of the mandible. II. Br J Oral Surg 1965;3(2):77–91. Crossref
-
Freedman GL, Beigleman MB. The traumatic bone cyst: a new dimension. Oral Surg Oral Med Oral Pathol 1985;59(6):616–18. Crossref
-
Boyne PJ. Treatment of extravasation cysts with freeze-dried homogenous bone grafts. J Oral Surg (Chic) 1956;14(3):206–12.
-
Whinery JG. Progressive bone cavities of the mandible: a review of the so-called traumatic bone cyst and a report of three cases. Oral Surg Oral Med Oral Pathol 1955;8(9):903–16. Crossref
-
Wong-Romo G, Carrillo-Terán E, Ángeles-Varela E. Solitary mandibular bone cyst. Case report and literature review. Quiste óseo solitario mandibular. Reporte de un caso y revisión de la literature. Rev Odont Mex 2016;20(2):114–22. Crossref
-
You MS, Kim DY, Ahn KM. Surgical management of idiopathic bone cavity: case series of consecutive 27 patients. J Korean Assoc Oral Maxillofac Surg 2017;43(2):94–9. Crossref
-
Saldaña SA, Gómez PBA, Díaz CR, Castillo GH. Maxillary and mandibular solitary bone cyst. Case report and literature review. Revista Odontológica Mexicana 2018;22(1):39–44.
-
Tymofieiev OO. Manual of maxillofacial and oral surgery [Russian]. 5th ed. Kyiv, Ukraine: Chervona Ruta-Turs; 2012.
-
Olvi LG, Lembo GM, Velan O, Santini-Araujo E. Simple bone cyst. In: Santini-Araujo E, Kalil R, Bertoni F, Park YK, eds. Tumors and tumor-like lesions of bone. 1st ed. London: Springer; 2015:611–33. Crossref
-
Lokiec F, Wientroub S. Simple bone cyst: etiology, classification, pathology, and treatment modalities. J Pediatr Orthop B 1998;7(4):262–73.
-
Xanthinaki AA, Choupis KI, Tosios K, Pagkalos VA, Papanikolaou SI. Traumatic bone cyst of the mandible of possible iatrogenic origin: a case report and brief review of the literature. Head Face Med 2006;2:40. Crossref
-
Demirbas AE, Colpak HA, Kutuk N, Gonen ZB, Alkan A. Analysis of traumatic bone cyst of the jaws: a retrospective study. Meandros Med Dent J 2019;20(3):225–9. Crossref
-
Resnick CM, Dentino KM, Garza R, Padwa BL. A management strategy for idiopathic bone cavities of the jaws. J Oral Maxillofac Surg 2016;74(6):1153–8. Crossref
-
Martins-Filho PR, Santos Tde S, Araújo VL, Santos JS, Andrade ES, Silva LC. Traumatic bone cyst of the mandible: a review of 26 cases. Braz J Otorhinolaryngol 2012;78(2):16–21. Crossref
-
Velasco I, Cifuentes J, Lobos N, San Martín F. The unusual evolution of a simple bone cyst in the mandible: a case report. J Clin Exp Dent 2012;4(2):e132–5. Crossref
-
Matsuda S, Yoshimura H, Sano K. A floating inferior alveolar neurovascular bundle in a simple bone cyst: A case report. Exp Ther Med 2019;17(6):4677–80. Crossref
-
Chell M, Idle M, Green J. Case report: an unusual finding of a solitary bone cyst in a patient with a fractured mandible. Dent Update 2015;42(10):977–8. Crossref